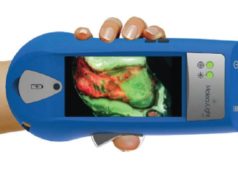
 Fluorescence imaging using the MolecuLight i:X can rapidly detect Pseudomonas aeruginosa (PA) in common wounds, a new study published in Diagnostics confirms. PA is a common bacterial pathogen in wounds known for its propensity to form biofilms and evade conventional treatment methods.
Fluorescence imaging using the MolecuLight i:X can rapidly detect Pseudomonas aeruginosa (PA) in common wounds, a new study published in Diagnostics confirms. PA is a common bacterial pathogen in wounds known for its propensity to form biofilms and evade conventional treatment methods.
The investigators conducted this independent, prospective clinical trial of 28 wounds as theearly detection of PA in wounds is critical to mitigate more severe wound outcomes.They explain that PA in wounds is associated with rapid wound deterioration, higher rates of skin graft failure, and higher rates of sepsis.
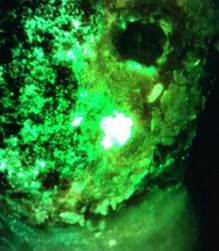
In the study, chronic wounds in which cyan was observed had tissue samples taken for culture analysis. Results of this analysis reveal that the cyan fluorescence detected in MolecuLight i:X images was predictive of PA in 93% of study wounds, yet less than 20% of the wounds exhibited the “classic” symptoms of Pseudomonas.
“I see non-healing wounds every day and struggle because the cause is often unclear. The ability to screen patients’ wounds on the spot and differentiate wounds harbouring Pseudomonas is a substantial clinical advantage that enables me to adjust therapy immediately”, says Rose Raizman, lead author of the study and wound care specialist at Scarborough Health Network, Lawrence S Bloomberg Faculty of Nursing at the University of Toronto (Toronto, Canada). “The study’s findings and my clinical experience with the MolecuLight i:X suggest that cyan detected on fluorescence images can be used to reliably predict Pseudomonas at the point-of-care”.
The need for definitive methods to improve bacterial detection in wounds at point-of-care is “indisputable”, given that >80% of wounds with high bacterial loads are missed by routine assessment, a MolecuLight press release states. The company continues: “The pathogenicity of PA and its propensity for biofilm formation make its rapid detection critical. Clinical guidelines advise use of clinical signs and symptoms to aid in the early detection of PA; however, these symptoms frequently fail to mount in infected wounds. Indeed, in this study, less than 20% of wounds that were positive for PA exhibited these symptoms. As such, clinicians may be missing the majority of wounds containing PA. This study illustrates how point-of-care fluorescence imaging, alongside assessment of clinical signs and symptoms of infection, may help to overcome these challenges. Fluorescence imaging potentially enhances detection of PA in wounds and also provides real-time information to wound care clinicians related to the efficacy of treatments targeted to eradicate PA.”